For Patients
Forms, brochures and all the information you need as a patient of our clinic.
FIND OUT MORECustomer Care
Our team of friendly staff are on hand to help you with all your clinical questions.
GET IN TOUCHDr Paul Cozzi offers a comprehensive Urological practice specialising in the treatment of prostate, kidney, testicular and bladder cancers, incontinence, erectile dysfunction, kidney stones, benign prostatic hyperplasia and infertility.
Why you should choose Dr Cozzi…
Cancer Control for Dr Cozzi’s patients is clearly better, as demonstrated by an independent audit performed each year.
One very important indicator of a surgeons ability to cure prostate cancer is the percentage of patients who have positive surgical margins at the time of surgery. A positive margin is defined as cancer cells present on the inked margin of the prostate under the microscope, and is dependant on the skills of the surgeon and the nature and extent of the cancer at the time of surgery.
A robotic prostatectomy audit for the 2019 calendar year reveals a positive surgical margin rate for Dr Cozzi, of 7.8% compared to the average across the state of 14.7%. This indicates that Dr Cozzi achieves a higher cure rate – as his patients can expect a positive surgical margin rate of less than half of his peers.
Book an appointment with one of the most experienced robotic urological surgeons in Australia in both UroLift and Rezum procedures.

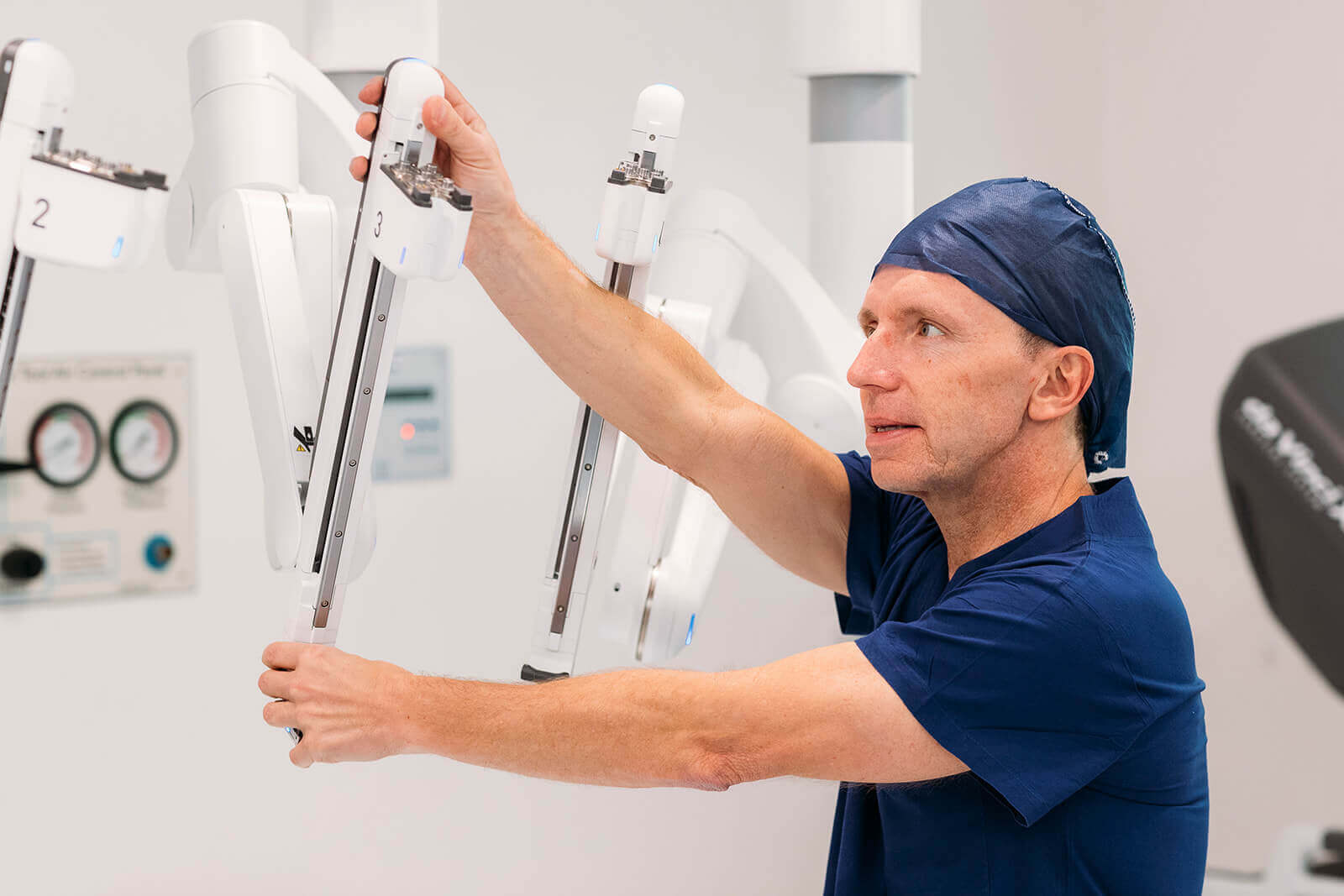
Robotic Urological Surgeon
Dr Cozzi has access to DaVinci Xi and DaVinci Si platforms available in Sydney at two leading private hospitals. With the latest and most advanced technology, outcomes for cancer control, and recovery of urinary continence and erectile function, can be optimised.

Prostate and Kidney Cancer Expert
Dr Paul Cozzi is internationally trained and recognised allowing his team to offer the best treatments for all stages of prostate cancer. His multidisciplinary unit incorporates the best medical oncology and radiation oncology to complement surgery available, to offer patients comprehensive cancer care.
Treatments & Procedures
Dr Cozzi was the first surgeon in Australia to be fully credentialed to perform water vapour therapy independently and currently offers the procedure to suitable patients each week with timely availability.
The operation to remove prostate cancer is called a “radical” prostatectomy, or, more properly, a total prostatectomy. This article is written to provide you with answers to the questions many patients and their families ask about the operation.
Penile implants involve the surgical insertion of malleable or inflatable tubes into the penis. A semi-rigid prosthesis is a silicon-covered flexible metal rod. Once inserted, it provides the rigidity necessary for intercourse and can be curved slightly for concealment.
Focus shockwave therapy is a non-invasive treatment that uses low-frequency, acoustic shock waves generated via a handheld device to improve blood flow to the penis and improve erection quality.